The HPV Vaccine Is Working: Rates Have Dropped Over 50 Percent Since Introduced
Though only half of teen girls have gotten one dose of the vaccine and fewer than a third have gotten the recommended three doses, new research has found that the proportion of teen girls infected with the strains of HPV that the vaccine addresses has dropped by 56 percent.
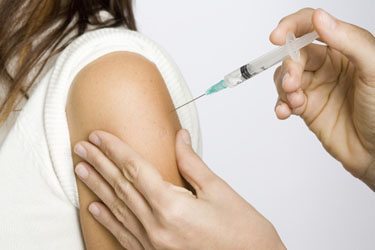
New research published in the Journal of Infectious Diseases shows that the human papillomavirus (HPV) vaccine, which has been controversial since even before Gardasil was approved by the Food and Drug Administration in 2006, is working. Despite the fact that only one half of teen girls have gotten one dose of the vaccine and fewer than one-third have gotten the recommended three doses, the proportion of teen girls infected with the strains of HPV that the vaccine addresses has dropped by 56 percent.
HPV is a highly contagious sexually transmitted disease (STD) that is spread from infected skin to uninfected skin. Transmission of HPV can be prevented by condoms, but only if the infected skin is in an area covered by the condom. If it is on an area such as a man’s scrotum, condoms cannot help reduce transmission.
Approximately 79 million Americans are currently infected with HPV, and about 14 million people become newly infected each year. HPV is so common that nearly all sexually active men and women will get at least one type of HPV at some point in their lives. Most of them will have no symptoms or health problems. In fact, the body can often clear itself of the infection without intervention. Some people, however, will get genital warts, which may go away on their own or may need to be removed by a health-care provider. Of greater concern is that certain strains of the virus, if left untreated, can lead to cervical cancer. Approximately 12,000 women in the United States are diagnosed with cervical cancer each year, and about 4,000 die. HPV can also cause cancer of the penis and anus, and is responsible for a recent increase in cases of head and neck cancers.
Gardasil was designed to provide protection against four common strains of the virus—the two that account for 70 percent of cervical cancers and the two that account for 90 percent of genital warts. (A second vaccine, called Cervarix, which only protects against the two strains that cause cervical cancer, was approved in 2009, but the authors of the study say that based on the timing of their data the effect is mainly a result of Gardasil.)
The vaccine is given as a series of three shots and is approved for young people—both men and women—between the ages of nine and 26. The Centers for Disease Control and Prevention (CDC) recommends that HPV vaccines become part of the routine vaccinations for girls who are 11 or 12 years old because in order to ensure that it works, it has to be given before they become sexually active. Though not recommended as part of the routine vaccinations for boys, health-care providers suggest that they receive the vaccine at the same age.
The current study was conducted by the CDC and compared infection rates in girls ages 14 to 19, before the vaccine was introduced and after. It looked specifically at those strains of HPV targeted by Gardasil. The proportion of girls infected with these dropped from about 12 percent before the vaccine was available to 5 percent (again, a drop of 56 percent). This applies to all teens, whether or not they were vaccinated. This may be a result of what public health experts refer to as “herd immunity”—if enough of the population is protected by a vaccine, that protection extends to the unvaccinated as well. Among girls who had gotten the vaccine, however, the drop in HPV infections was even higher, at 88 percent.
The study did not look at rates of cervical cancer, but since that disease develops so slowly, it is unlikely that the vaccines have had an impact on rates yet.
The study also found that the proportion of teens who had ever had sex did not go up, nor did the proportion of those who had had multiple sex partners. This should not be surprising, as other studies have also found that access to the vaccine does not give young people license to engage in unsafe sexual behavior, as opponents of the vaccines have argued. (See this Rewire article for further discussion on this argument). The study did find that a higher percentage of vaccinated teens said they’d had three or more sex partners. Dr. Lauri Markowitz, the study’s lead author, told the Washington Post this suggested that those teens most in need of the vaccine’s protection were getting it, and that by preventing the virus in them, their peers were protected as well.
One interesting result of this study is that the protection seems to have set in even though so few teens have had the recommended three doses of the vaccine. Markowitz said this warranted further study and discussion about whether all three shots are necessary.
