This Week in Sex: News From the HIV Epidemic
This week in sex: Scientists report the first case of HIV transmission to a patient adhering to PrEP protocols, two studies show a new vaginal ring can help women prevent HIV, and young people still aren't getting tested for the virus.
This Week in Sex is a weekly summary of news and research related to sexual behavior, sexuality education, contraception, STIs, and more.
With the death of Nancy Reagan, the 1980s AIDS crisis is back in the national spotlight. But, of course, HIV and AIDS are still ongoing problems that affect millions of people. This week in sex, we review scientists reporting the first case of HIV transmission to a patient adhering to PrEP protocols, two studies showing a new vaginal ring can help women prevent HIV, and evidence that young people still aren’t getting tested for the virus.
First Case of HIV Transmission While on Truvada
Last week, Canadian scientists reported on what they believe to be the first HIV infection in a patient who was following a PreP (Pre-Exposure Prophylaxis) regimen.
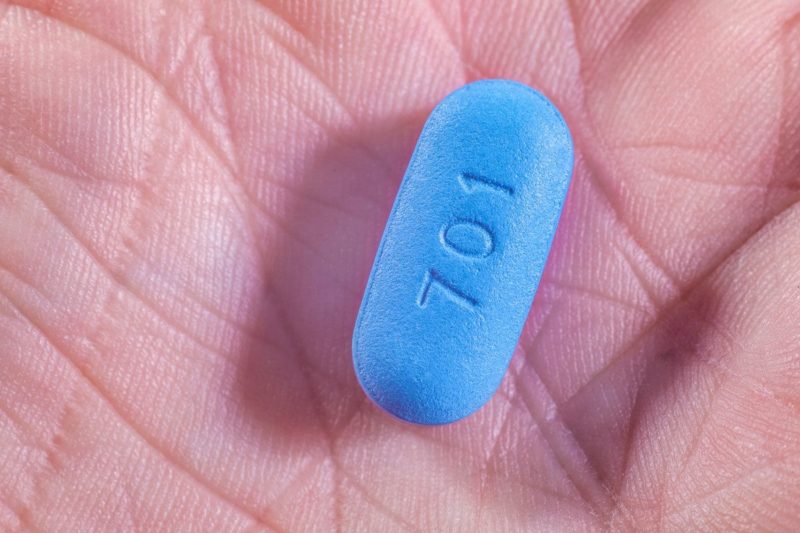
PrEP is a method of HIV prevention. By taking a daily pill that contains two HIV medicines, sold under the name Truvada, individuals who are HIV-negative but considered to be at high risk of contracting the virus can prevent infection. Studies have found that PrEP is very effective—the Centers for Disease Control and Prevention estimates that people who take the medication every day can reduce their risk of infection by more than 90 percent from sex and by more than 70 percent from injection drug use. One study of men taking PrEP found no infections over a two-and-a-half-year period.
PrEP is less effective when not taken regularly, but the new case of reported PrEP failure involves a 43-year-old man who said that he took his medication daily. His pharmacy records back up that assertion. The man’s partner has HIV, but is on a drug regimen and has an undetectable viral load. The man did report other sexual encounters without condoms with casual partners in the weeks leading up to his diagnosis.
Dr. David Knox, the lead author of this case study, notes that it is difficult to know if a patient really did adhere to the drug regimen, but the evidence in this case suggests that he did. He concluded, “Failure of PrEP in this case was likely due to the transmission of a PrEP-resistant, multi-class resistant strain of HIV 1.”
Experts say, however, that they never expected PrEP to be infallible. As Richard Harrigan of the British Columbia Center for Excellence in HIV/AIDS told Pink News, “I certainly don’t think that this is a situation which calls for panic …. It is an example that demonstrates that PrEP can sometimes be ineffective in the face of drug resistant virus, in the same way that treatment itself can sometimes be ineffective in the face of drug resistant virus.”
Still, some fear that the new study will add to the ongoing debate and apathy that seem to surround PrEP. While some experts see it as a must-have prevention tool, others worry that it will encourage men who have sex with men to forgo using condoms and perhaps increase their risk for other sexually transmitted infections. Still, only 30,000 people in the United States are taking the drug—an estimated one-twentieth of those who could benefit from it.
A New Vaginal Ring Could Help Women Prevent HIV Infection
Researchers have announced promising results from two studies looking at new technology that could help women prevent HIV. The dapivirine ring, named after the drug it contains, was developed by the International Partnership for Microbicides. It looks like the contraceptive ring, Nuvaring, and is similarly inserted high up into the vagina for a month at a time. Instead of releasing hormones to prevent ovulation, however, this ring releases an antiretroviral drug to prevent HIV from reproducing in healthy cells. (A ring that could prevent both pregnancy and HIV is being developed.)
The two studies of the ring are being conducted in Africa. One study recruited about 2,600 women in Malawi, South Africa, Uganda, and Zimbabwe. It found that the ring reduced HIV infection by 27 percent overall and 61 percent for women over age 25. The other study, which is still underway, involves just under 2,000 women in seven sites in South Africa and Uganda. Early results suggest that the ring reduced infection by 31 percent overall when compared to the placebo.
Both studies found that the ring provided little protection to women ages 18-to-21. Researchers are now working to determine how adherence and other biological factors may have impacted such an outcome.
Young People Not Getting Tested for HIV
A study in the February issue of Pediatrics found that HIV testing rates among young people have not increased in the last decade. The researchers looked at data from the Youth Risk Behavior Survey (YRBS), which asks current high school students about sexual behaviors in addition to questions about drugs and alcohol, violence, nutrition, and personal safety (such as using bike helmets and seat belts). Specifically, the YRBS asks students if they’ve ever been tested for HIV.
Using YRBS data collected between 2005 and 2013, the researchers estimated that 22 percent of teens who had ever had sex had been tested for HIV. The percent who had received HIV tests was higher (34 percent) among those who reported four or more lifetime partners. Overall, male teens (17 percent) were less likely than their female peers (27 percent) to have been tested.
Researchers also looked at data from the Behavioral Risk Factor Surveillance System, which asks similar questions to young adults ages 18 to 24. Among people in this age group, between the years of 2011 to 2013, an average of 33 percent had ever been tested. This review of data also found that the percentage of young women who get tested for HIV has been decreasing in recent years—from 42.4 percent in 2011 to 39.5 percent in 2013.
The authors simply conclude, “HIV testing programs do not appear to be successfully reaching high school students and young adults.” They go on to suggest, “Multipronged testing strategies, including provider education, system-level interventions in clinical settings, adolescent-friendly testing services, and sexual health education will likely be needed to increase testing and reduce the percentage of adolescents and young adults living with HIV infection.”
